Ntension typically plays to a crowd.The Hermon-based company specializes in large-scale tension-fabric structures for trade shows and exhibits, elaborate temporary construction designed to draw attention and draw people in. Not in 2020.
As the pandemic forced the cancellation of the big events that make up Ntension’s regular market, the company, with help from the University of Maine, began exploring products with a much smaller footprint: personal protective equipment (PPE) for health care workers.
Leveraging its existing fabric manufacturing capacity, Ntension moved ahead deliberately, first working with UMaine’s Advanced Manufacturing Center (AMC) last spring to test the filtration properties of materials that could be used to make face masks.
From there, the company began production of face masks and shields, working closely with Northern Light Health to meet the medical group’s specifications for a general-use mask that could be worn by those whose duties don’t require an N95. Ntension is in the early stages of developing a medical product line, and has continued to work with AMC on product development and process improvements as it begins to build capacity and pursue U.S. Food and Drug Administration (FDA) approval for their masks.
As AMC director, John Belding regularly visits Maine manufacturing company sites to assess operational effectiveness, plan prototype projects and help link UMaine research with industrial needs.
AMC’s work with Ntension is one example of statewide economic development efforts during the pandemic. Indeed, partnerships between the engineering support and service center and manufacturers throughout Maine have been more important than ever in addressing COVID-19-related challenges.

Since late summer, Belding’s focus has been on asking detailed questions about operations and gathering data for a sweeping project aimed at helping Maine’s manufacturing sector weather the ongoing economic effects of the pandemic.
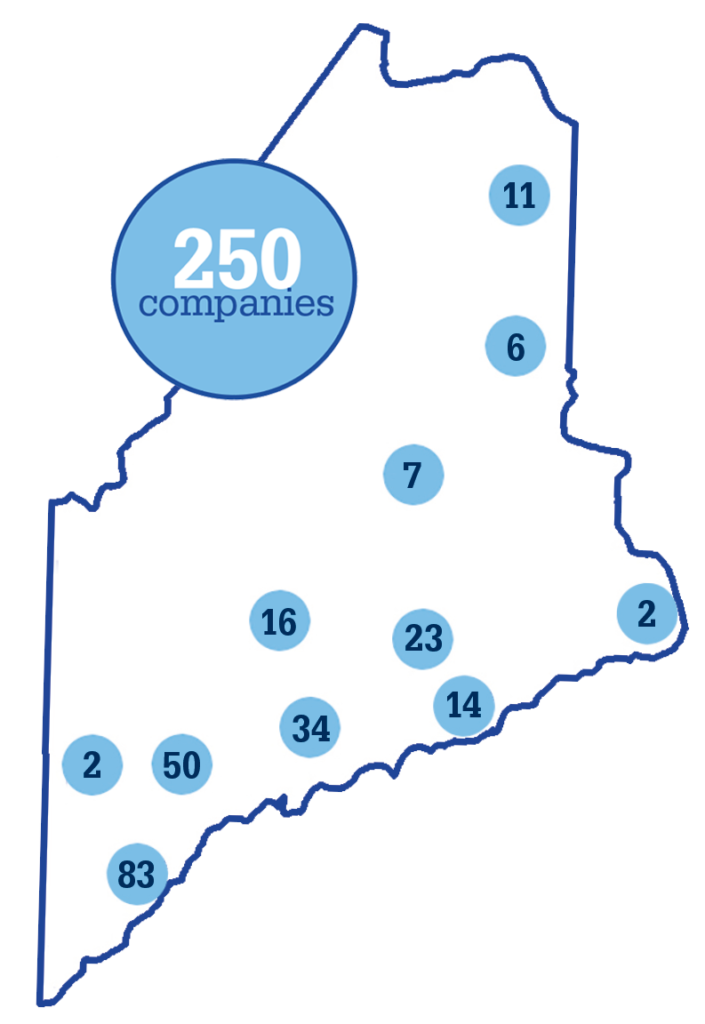
The COVID Countermeasures Project is a collaborative effort that marries AMC’s product and process development and research with services provided by the Maine Manufacturing Extension Partnership (Maine MEP) and the Manufacturers Association of Maine (MAME), two regional trade organizations. Supported by $286,000 in CARES Act funding and a $100,000 grant from the Maine Technology Institute, they surveyed more than 250 companies about impacts related to the pandemic and are conducting 50 in-depth assessments for companies that requested additional support. From these assessments, the group is developing a series of customized remediation projects to solve individual challenges.
It’s a big lift for a critical sector that accounts for more than 54,000 Maine jobs and a $5.9 billion share of the state’s gross domestic product. Projects run the gamut from marketing assistance to engineering work, and draw on the expertise of a statewide network of consultants, including AMC.
“Basically, we can do anything,” Belding says of the collaborative. “It’s a great partnership that builds on company retention work MAME was already starting to do. Responding to COVID has reinforced the purpose. By pooling our resources and our expertise, we’ve been able to develop a well-defined plan for how to approach this.”
Some firms the group works with are trying to make existing processes more efficient. Others, such as Ntension, have ventured into entirely new markets as a result of COVID.
Months into a public health crisis that has upended life in Maine and across the world, the COVID Countermeasures Project is an active example of UMaine’s ongoing response efforts. While the pace has shifted from the frenzied early days of the pandemic, the university’s role and mission to support evolving state needs remain unchanged.
In the beginning
In the first week of March, professor of chemical and biomedical engineering Mike Mason received an urgent email from one of his regular contacts at Northern Light Eastern Maine Medical Center in Bangor.
“The message essentially said ‘We’re exploring strategies to continue to supply critical PPE, and we’d like some help troubleshooting on different sterilization strategies we might use,’” Mason says.
Mason talked regularly with the sender, Northern Light Health director of clinical engineering Ken Mitchell, but their discussions typically revolved around student projects related to UMaine’s biomedical engineering co-op program. As COVID-19 spread rapidly worldwide and began appearing in New York and Boston, the conversation was very different.
On March 3, 2020, the World Health Organization (WHO) warned of severe and mounting disruption to the global supply of PPE. Northern Light EMMC, like many other hospitals, began investigating all options to keep its staff safe.
“My first thought was that this was a problem that we might be able to help with, but I was also not fully aware yet how seriously COVID was impacting the health care supply chain,” Mason says. “That is to say, the normal inventory of supplies was not going to cut it because the daily burn rate for these things is huge.”
Mitchell’s email set in motion UMaine’s research response to COVID-19, spawning the development of a broad-based COVID-19 innovation team that brought together multiple university research centers, and representatives from Maine health care, manufacturing and government to solve emerging challenges related to the pandemic. The UMaine-led group tackled PPE needs from hand sanitizer to ventilator parts, working swiftly to address problems the state was facing and initiating collaborations that would reach far beyond the campus.
Bringing people together
Mason and Mitchell began talking through potential sterilization strategies for N95 masks. By the second week of March, other faculty members in the department — including assistant professor of chemical and biomedical engineering Caitlin Howell and professor of practice Robert Bowie — were approached by their own contacts at area hospitals, many of them raising similar issues.
“We were hearing about masks, face shields, ventilators and ventilator parts — vent pieces and splitters — and we didn’t have good clarity on what the need was going to be yet,” says Mason. “It was everything from ‘We’re not going to need much’ to ‘We’re going to need a thousand of these a day and how fast can you make them?’
“It started to become obvious that we were all dealing with different aspects of the same problems, but not really making a lot of progress,” says Mason. “We needed to organize.”
To coordinate that process, Mason called on Jake Ward, UMaine vice president of innovation and economic development, and noted coalition builder.
“Mike told me what he was hearing from the hospitals and we just started bringing people in on the different issues,” says Ward. “In the beginning, it all seemed to center around what we might be able to 3D print. But we realized that first we needed to understand the hospitals’ needs to make sure we were producing items that were needed and could actually be used in a medical setting.”
The first formal meeting of what would become the COVID-19 innovation team occurred March 19. Ward invited experts from across the university and the state, and encouraged them to invite others.
A broad-based COVID-19 innovation team brought together multiple university research centers and representatives from Maine health care, manufacturing and government.
“I think we had 47 people on the first call,” Ward says. “The working relationships I and others already had with all those individuals made it easy to pull that group together, and using Zoom, allowed us to assemble people from all over the state in a short time. We had people who never came back again, and went off and worked on different issues independently, but the group that stuck was one that wanted to be interdisciplinary and work together.”
That unit eventually gelled to include faculty, staff and students, representatives from the Maine Department of Economic and Community Development, Maine MEP, MaineHealth, St. Joseph Hospital, and Northern Light Health. Other collaborating partners included MAME and Maine Procurement Technical Assistance Center.
Those early days were a blur of activity. And daily calls. Ward opened the discussion the same way — by asking the participating members of the medical community what they were hearing, what they were seeing and what they needed.
“We were talking a lot about masks, but part of that conversation was ‘Are there other things that you guys are running out of?’” says Mason. “And that’s when we first heard about sanitizer.”
It was the end of the third week of March. Shortages that had been looming began to take on new urgency as the pandemic took hold nationwide and hospitals’ regular supply chains were increasingly strained by high demand.
“I believe it was on that Friday the 20th that we got connected with Central Maine Medical Center,” Mason says. “And they said, ‘We’re not only looking at a problem, we’re out on Sunday.’”
Getting started
The pressing need for hand sanitizer kicked UMaine’s response into high gear. The Department of Chemical and Biomedical Engineering team took the lead on the project, reaching out to hospitals statewide to coordinate with their in-house pharmacists about the required formulation for hand sanitizer.
Mason enlisted the help of two of his graduate students, Aileen Co and Radowan Hossen, to broadcast a list of needed supplies to the campus research community, and the response was swift.
“People gave us glycerin and hydrogen peroxide from their labs,” says Mason. “We didn’t know at first how much we were going to need and the idea was that if we could just get 25 gallons of the stuff made, it would help us prove the process and meet that need for Central Maine.”
Mason spent Friday and Saturday nights poring over documentation on formulas provided by the hospitals, FDA and WHO. March 22, he and professor William DeSisto met at the Process Development Center (PDC) in Jenness Hall, ready to go to work.
“We did a little chemistry,” Mason says. “What we found is that it’s really easy to make. It’s a liquid hand sanitizer, not gel, so it’s not very complex in terms of mixing.”
The 25-gallon pilot batch of FDA-compliant, hospital-grade, 80% ethanol hand sanitizer was distributed to Central Maine Medical Center in Lewiston and Northern Light EMMC in Bangor that same day, meeting urgent needs.
“By the end of the weekend, we thought ‘Hey, this is really something we can do, but we don’t have enough ethanol. How can we get that one critical component, and how do we go about tapping into the available supply chain to get the other things that we need?’”
Scaling up to meet demand
At this point, Ward’s rapid innovation collaborative concept began to crystallize. The group kept the “fail fast, fail cheap” principle of innovation front of mind as it looked for solutions to supply chain issues.
“If hand sanitizer is a product we need to produce, how are we going to get legal on board, can we set up an account to buy materials, how do we do that?” Ward says. “The work we do in the Department of Industrial Cooperation made it easy for us to facilitate that interaction and help get things done within the university.”
The team operated as part of a March 22 agreement with the Maine Emergency Management Agency (MEMA), allowing the University of Maine System to provide goods and services to state health care facilities and agencies.
While the first batch of sanitizer marked a milestone, the work was just beginning. With supplies increasingly tight, the team realized that an intricate understanding of hospital demand was critical to the success of hand sanitizer and any other potential projects. Rapidly changing FDA guidance was another reality for both the team trying to find solutions and the health care facilities trying to respond.
“The hospitals can’t decide to use something just because they have it,” says Mason. “We knew that things the FDA would never approve weren’t true solutions, but we also knew we had this industrial production capacity if we could identify the right items.
“We also had to translate the way the hospitals were used to ordering supplies into a daily burn rate that we could use to gauge production,” says Mason. “With hand sanitizer, we knew we couldn’t deliver a thousand gallons tomorrow, but we could deliver 50 gallons a day for 20 days. Really understanding the actual supply chain requirement became so important that we had to start putting people on just that.”
Once word got out that UMaine could make hospital-grade hand sanitizer, demand from medical facilities intensified. Mason and his collaborators began fielding hundreds of emails per day on the subject and Mason tapped his graduate students to coordinate with hospitals about their needs. Managing logistics essentially became a full-time job for Co, a biomaterials engineering Ph.D. student, who was among those in the UMaine community putting in 14-hour days.
The project scaled up and soon the university’s hand sanitizer production was being run out of PDC, UMaine’s commercial-scale pilot plant that supports the pulp, paper and bioproducts sector with research, development, demonstration and commercialization services. With its existing capacity for commercial-scale products and chemical engineering processes, the facility was able to pivot swiftly to scale up production in early April. The PDC staff’s logistics expertise also proved to be an asset in coordinating the supply of ethanol and other materials, a persistent challenge in the operation’s early days.
Working in 50-gallon batches, PDC shipped more than 3,000 gallons of hand sanitizer to more than 100 locations in Maine. Recipients included major hospitals, long-term care facilities, Maine tribal health facilities and first responders.
“It was a mad scramble to get materials,” says PDC director Colleen Walker. “In the beginning, we estimated we might need to make 190 gallons per day, and we were thinking ‘Where the heck are we going to get the alcohol?’”
The answer came from Maine’s craft distilleries and brewers, largely idle after the state’s restaurants and bars closed March 18.
Mason and Walker began working with the Maine Distillers Guild to source ethanol, including some made from local brewers’ unsold beer, to support hand sanitizer production. New England Distilling, Hardshore Distilling, Stroudwater Distillery, Sebago Lake Distillery, Split Rock Distilling, Blue Barren Distillery and Mossy Ledge Spirits were among the university’s partners in this effort, and brewers including Allagash, Maine Beer, Rising Tide, Foundation, Oxbow, Shipyard and Baxter provided feedstock for the distilleries. A sizable donation of high-proof alcohol from Boston Brands of Maine also supported early UMaine efforts.
“UMaine was the guiding hand to give us direction for this effort,” says Ned Wight, president of the guild and one of the owners of the Portland-based New England Distilling. “First, working with the university allowed us to contribute alcohol and do it legally. Second, they had the manufacturing and supply connections to procure the other chemicals that were needed and handle compounding, packaging and distributing the sanitizer to hospitals, which allowed us to focus on what we know how to do — the alcohol side.”
Extracting the ethanol for delivery to UMaine was no small feat. Wight’s operation and others collectively distilled approximately 20,000 gallons of beer that otherwise would have been discarded.
The sheer volume of alcohol involved required PDC to get some special permissions.
“We had to get approval from the town of Orono to have so much alcohol on site, and the fire department to work with the alcohol inside the building,” says Walker.
The biggest shift, Walker says, was adjusting the pace of PDC’s operations and coordinating the many individual steps in the process, from procuring the alcohol to working with UMaine Facilities Management to ensure delivery of the final product. Health care facilities were able to place orders through the WebEOC, a communications system used in state emergency operations. Co responded to each request, tracking packaging requirements and other details that PDC staff used to build a production schedule. Once an order was complete, Facilities Management arranged delivery.
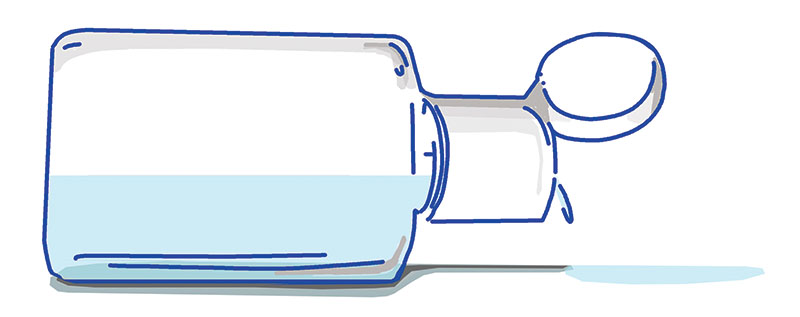 Working in 50-gallon batches, PDC shipped more than 3,000 gallons of hand sanitizer to more than 100 locations in Maine. Recipients included major hospitals, long-term care facilities, Maine tribal health facilities and first responders.
Working in 50-gallon batches, PDC shipped more than 3,000 gallons of hand sanitizer to more than 100 locations in Maine. Recipients included major hospitals, long-term care facilities, Maine tribal health facilities and first responders.
Parallel projects
While hand sanitizer production and coordination emerged as the signature piece of UMaine’s response to meet state needs in the pandemic, it was not the only initiative members of the innovation team tackled. Projects emerged rapidly and with much still unknown about how severely the virus would impact Maine, there was a lot on the table.
The Advanced Manufacturing Center, home to an engineering support and resource center specializing in precision manufacturing, played a key role in several of these projects, including design, prototyping and materials testing services for a variety of companies looking to respond to shortages and emerging needs.
AMC’s work started with an early effort to develop masks that could be manufactured in state for use in a medical setting to answer PPE shortages. While that project ultimately did not move forward, a number of Maine companies began making cloth face coverings for consumer use.
The AMC team, led by Belding, tested in excess of 100 different types of material intended for use in face coverings, everything from basic cotton T-shirts to technical fabrics. Their methods measured how effective the material is at blocking particles of different sizes.
While no certified protective face masks for hospital use are currently being manufactured in Maine, AMC helped a number of companies, including L.L. Bean and Strainrite, gauge the filtration properties of different types of material they explored for use in face coverings. AMC has continued work with Ntension as the Hermon firm cultivates PPE product lines and pursues medical certification.
In a similar vein, the center tested N95 masks before and after different sterilization treatments to ensure the filtering performance was not degraded, supporting hospitals’ exploration of techniques to allow for limited reuse of PPE.
AMC also assisted Maine plastics manufacturers with new products. Given nationwide shortages of N95s, many hospitals turned to alternative forms of PPE, including clear plastic face shields intended as an extra layer of protection. The shields made an ideal product for local manufacture, and AMC facilitated their rapid development by evaluating prototype designs.
By late April, Maine companies had produced hundreds of thousands of shields, more than enough to meet in-state needs and supply other markets.
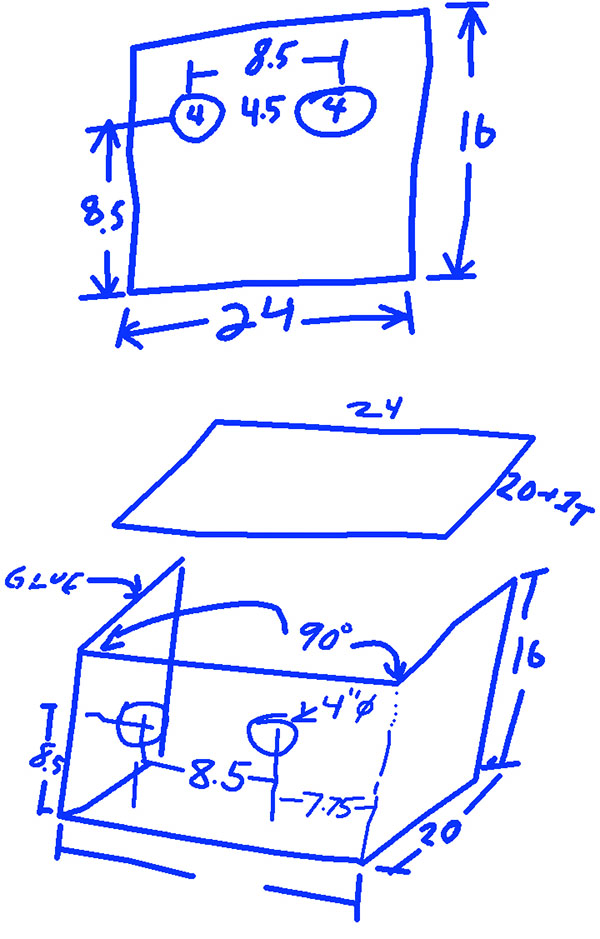 A request from MaineHealth led to AMC prototyping two designs for “aerosol boxes” that can be used to protect medical workers during transportation and intubation procedures in patients suspected to have COVID-19. The designs are based on a concept first conceived by Dr. Hsien- Yung Lai, a physician in Taiwan whose aerosol box design to treat COVID-19 patients has been shared widely during the pandemic.
A request from MaineHealth led to AMC prototyping two designs for “aerosol boxes” that can be used to protect medical workers during transportation and intubation procedures in patients suspected to have COVID-19. The designs are based on a concept first conceived by Dr. Hsien- Yung Lai, a physician in Taiwan whose aerosol box design to treat COVID-19 patients has been shared widely during the pandemic.
AMC’s designs, developed in coordination with professor Bowie and with help from the Maine MEP, were tested in area hospitals and refined based on feedback from the front lines. The first is a three-sided shield, with handholes, that covers the patient’s head and shoulders, and allows medical personnel to intubate safely to contain aerosol spray from a patient’s respiratory tract. The second fully encloses a patient’s head and, with the help of a portable tube and filter, creates a negative-pressure environment so that viral particles leaving a patient’s respiratory tract can be captured to minimize contamination.
Both variations of the boxes were manufactured in Maine for Maine hospitals.
AMC also worked on ventilator parts and pieces, including a splitter that would allow two patients to share the same ventilator in the event of a shortage.
In late April, PDC also responded to an urgent request from Maine Center for Disease Control and Prevention (Maine CDC) for chemical solutions used to fit medical workers with N95 masks. There was a national shortage of fit-testing kits and test solutions.
Fit testing to ensure the seal between the facepiece on a respirator mask and the wearer’s face is required by the U.S. Occupational Safety and Health Administration. The test must be conducted when a worker is first fitted for a respirator, such as an N95. COVID-19 has created an expanded need for respiratory protections in health care and other settings, resulting in a surge in fit testing.
In May and June, UMaine delivered 4,500 bottles of fit-testing solutions for Maine CDC to distribute to the Maine National Guard and partner agencies that conduct the tests.
While the N95 is typically a single-use mask, hospitals began evaluating protocols to sterilize and reuse this and other forms of PPE in the face of shortages. Howell and professor David Neivandt have provided key counsel to Maine’s health care community on decontamination and sterilization of PPE.
At UMaine’s Virtual Environments and Multimodal Interaction (VEMI) Lab, staff and students led by director Richard Corey explored a range of technology projects, including the development of 3D-printed infrared thermometers that were in short supply and considered a potentially vital screening tool for businesses and schools. Using parts readily available for purchase online, the lab was able to design a nonmedical-grade thermometer that could be printed economically at home. The lab also released a guide to support hobbyists who might produce them for community use. In addition, VEMI served as a key resource for Maine officials exploring prospective COVID tracking apps and other potential software solutions.
“All these projects went off on their own tracks, but bringing everybody together (in daily virtual meetings) to hear the same things meant we could run things to ground really quickly with an understanding of the urgency from the front lines,” Ward says.
Reflecting
As the state’s flagship research university, UMaine had both the capability and the responsibility to respond in a crisis. The university-led innovation efforts established a new framework to address not only Maine’s worst-case COVID-19 scenarios, but a range of other challenges.
“We pulled this group together based on existing working relationships, but what it turned into was a function of the people who participated,” says Ward. “The diversity of the group made the difference because everybody had a chance to bring their lens to the issues, from health care to manufacturing to government to the different research groups on campus. If you’re really trying to solve problems, you need that kind of blend. You need to be able to think about quick answers, quick solutions that can help you rule things out. We just had a group of really pragmatic subject matter experts who were willing to listen to other subject matter experts, and it worked.”
For Mason and others who were part of the group, what emerged from the crisis was a common language that already is helping to support collaborations between the university, health care and other key sectors in Maine.
“In the beginning, translating the hospitals’ normal rate of purchasing supplies into what we could think of as a daily production rate was a significant hurdle,” says Mason. “We had all this capacity that we couldn’t engage until we found clarity, but once we truly understood the need, we could start providing solutions. From the very beginning, when we were staring the possibility of the worst-case scenario in the face, the professionals in the health care sector and the involved UMaine faculty did not panic, but got to work to meet a need that was a moving target the whole way. I think that building that trust and expanding those networks through this process will open the door to new conversations.”
This is already happening. Regional health care partners and UMaine have established a working group to apply rapid innovation principles to other public health challenges, such as addiction and rural access to care.
The collaborations forged and reinforced in the early days of the crisis have now shifted to meet longer-term needs for Maine businesses, such as the work AMC is doing to support manufacturers.
“We now have better, stronger relationships with the people we were already working with,” says Belding. “This COVID Countermeasures Project is one example of that. I think it helped broaden awareness of the university’s capabilities, too, and people understand that if other stuff comes up, we’ll be here to help.”
Ward, whose everyday role centers around emphasizing UMaine’s willingness and ability to problem solve to support state priorities, has found the process invigorating.
“I didn’t go into this thinking ‘What’s the machine that’s going to work and how are we going to make it?’” says Ward. “We were innovating the process, never mind the solutions.
“How can we apply the things we know now to what is happening around us? This effort showed the value of deploying our existing knowledge fairly quickly to help solve problems,” Ward says.
COVIDCountermeasures Project
Assessments and assistance for
businesses affected by COVID-19
Maine Manufacturing Extension Partnership
Manufacturers Association of Maine
University of Maine Advanced
Manufacturing Center